Neck pain is an incredibly common and potentially debilitating condition that ranges from mild to life altering. It can have many different sources including alterations to bones, discs, tendons, and muscles. Most of the time, neck pain is brought on by age-related changes in the discs and joints in the neck (called cervical spondylosis). Another name for it is arthritis of the neck. Unfortunately these changes are extremely common, with more than 85% of people over the age of 60 affected. Pain and stiffness are the most common symptoms but in several cases, individuals with arthritis in their neck experience no noticeable symptoms. Some good news to keep in mind is that neck pain typically responds very well to conservative measures. Lets review some basic anatomy before discussing details:
- The spine has 24 main bones called vertebrae, stacked on top of each other and separated by discs.
- There are seven vertebrae in the neck that comprise the cervical spine that begin at the base of the skull.
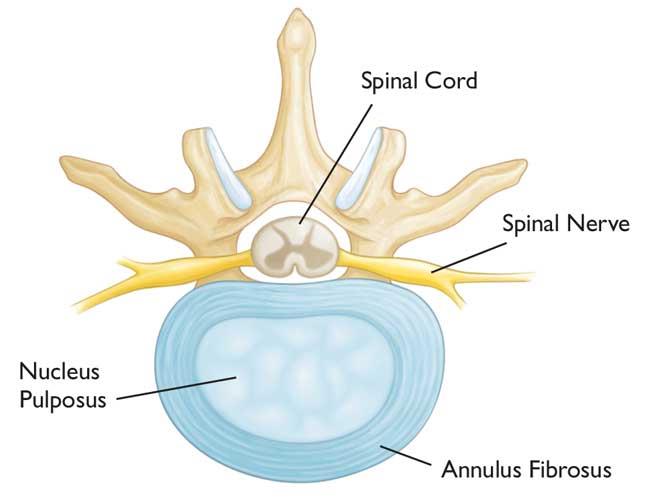
- The spinal cord and nerves act like “electrical cables” that carry messages to and from the brain. They travel in the spinal canal just behind the vertebrae, with the nerve roots branching out from the spinal cord and traveling to the extremities through channels between the vertebrae called “foramen”.
- The intervertebral discs between the vertebrae are meant to be flexible and can act like shock absorbers when you walk or run. They are made up of a tough, flexible outer ring called the annulus and a soft, jelly-like center called the nucleus pulposus.
- There are two small facet joints in the back of the spine at every level that connect the above and below vertebral bones.
Cause
Cervical spondylosis arises from degenerative changes that occur in the spine as we age. Most of these changes are normal, with nearly half of all middle-aged and older patients having worn out discs. Sometimes genetic pre-disposition can cause these changes to progress faster than in other people.
Disc Degeneration
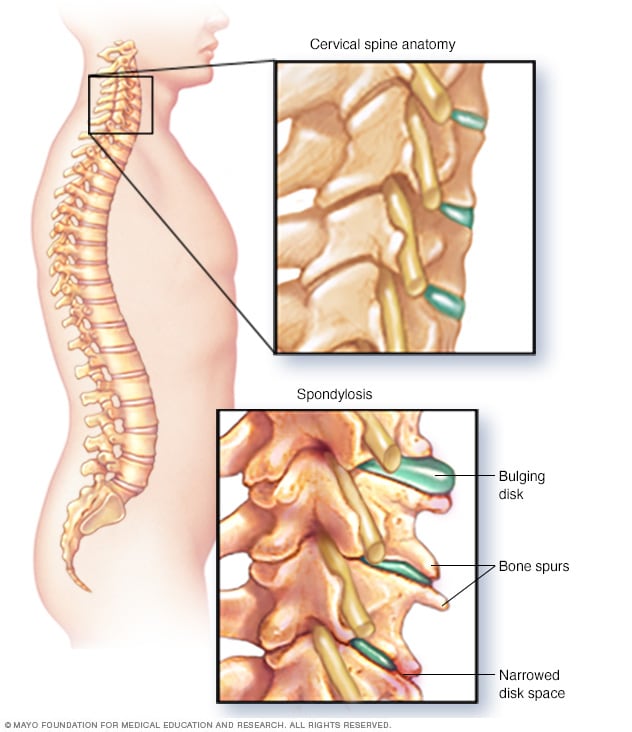
As the discs in the spine age, due to wear and tear as well genetic reasons, they can lose height and start to dehydrate, bulge out, and eventually weaken. This eventually causes settling or collapse of the disc space and as a result, more pressure gets placed on the small facet joints in the back. As these joints experience increased pressure, they can deteriorate and develop arthritis similar to the hip or knee. Once the smooth, slippery cartilage in the joints wears away, bone rubs on bone and can be painful and also stimulates the body into bony overgrowth creating “bone spurs”. Over time these bone spurs can narrow the space for the nerves to pass through their channels as well as for the spinal cord.
Risk Factors
Age is the biggest risk factor for developing degenerative changes in the cervical spine. Other factors can include a family history of similar neck issues, smoking, occupational hazards with repetitive motion and overhead work, depression and anxiety, or previous trauma or injury to the neck.
Symptoms
Symptoms of cervical spondylosis can vary greatly. For some it can cause no symptoms at all. When they do occur it can be in the form of pain and stiffness in the neck with motion or at rest. Pain can range from mild to severe in nature and sometimes can worsen with looking up or looking down. Other activities such as driving, reading a book, or working on a computer where your head stays in one position for a long time can also cause pain. Some other symptoms that can occur with cervical spondylosis are:
- Muscle spasms in the neck or shoulders
- A grinding or popping sensation when turning your head
- Headaches
If bone spurs and inflammation end up causing narrowing of the channels for nerves or the spinal cord then other conditions called radiculopathy or myelopathy could evolve. Symptoms could include pain, numbness, and weakness in the arms, hands or fingers. They could also include trouble walking, loss of balance, weakness in the hands or legs, or bowel/bladder dysfunction.
Workup
In order to properly evaluate neck pain your doctor should ask you specific questions to help him or her understand its nature. Some questions might pertain to when the pain started, when it usually occurs, what activities make it worse, what treatments you’ve had so far, or if you’ve ever been in an accident. In addition, a thorough physical examination is very helpful in understanding your condition. Specific areas that your doctor will look at for abnormalities are:
- Walking ability (gait)
- Reflexes
- Flexibility
- Sensation to touch in your arms
- Strength in your arms, hands and shoulders
Tests
There are specific tests that are helpful in determining the cause and degree of cervical spondylosis and the selection of them depend upon your individual symptoms. They may include:
- X-rays: These are very helpful in your workup and may be one of the first tests ordered. They show the bones in the spine very well and reveal whether there are any problems with degenerative changes (loss of disc height or bone spurs), alignment issues, or instability between bones like slippage forward or backward.
- Magnetic resonance imaging (MRI): This can be indicated if you have had several weeks of symptoms without improvement or worsening symptoms. Or can be obtained sooner if you have more of the concerning symptoms for nerve pinching listed above. These tests allow excellent visualization of the soft tissues in the body like your discs, nerves, and spinal cord. In conjunction with your history and physical exam, an MRI can help determine whether your symptoms are caused by a problem with any of these tissues.
- Computed Tomography (CT): These scans display structures similar to an X-ray but with more detail and with 3D visualization.
- Myelogram: This is a special type of CT scan where a contrast dye is injected into the spinal canal before the CT scan to allow the spinal cord and nerve roots to show up very clearly. You may need to get one of these if you have a pacemaker or other metal in your body preventing you from getting an MRI.
- Electromyography (EMG): This test measures the electrical activity inside of your muscles at rest and during contractions. This is helpful in the setting of multiple different degenerative findings on your MRI for example, in order to pinpoint a more specific nerve that could be causing the problem.
Treatments
In most cases, treatments for neck pain from cervical spondylosis is nonsurgical and usually very successful. There are multiple options for management and usually the best results will come from a combination of them specific to you. Treatments include:
- Physical Therapy (PT): PT is an excellent treatment for neck pain and spondylosis and will usually be one of the first treatment options pursued. Targeted exercises for neck muscle strengthening, stretching, and range of motion can help alleviate pain and maintain better posture. In some cases, posture therapy or gentle traction can also be helpful be reliving pressure on the joints and bones in the neck. PT programs vary in length and are specific to each patient but typically last anywhere from 6-8 weeks with sessions anywhere from 1-3 times per week.
- Medications: Several medications may be used alone or in combination to address pain and inflammation during exacerbations of your pain. These include acetaminophen for mild symptoms and nonsteroidal anti-inflammatories such as ibuprofen and naproxen which can relieve both pain and swelling. Muscle relaxants such as cyclobenzaprine can be used to treat painful muscle spasms if they occur. Rarely if ever should narcotic medication be used to manage symptoms as other complications and issues may occur from their long-term use.
- Ice, heat, and other modalities: Along with ice and heat, other modalities such as massage, acupuncture, and topicals can be effective at treating symptoms.
Steroid-based injections
Several patients find short and sometimes long-term pain relief from steroid-based injections performed by well-trained doctors. Although these options are less invasive than surgery, they should only be performed after a complete evaluation by your doctor as well as after discussing the risks and benefits as well as alternatives. The most common procedures utilized include:
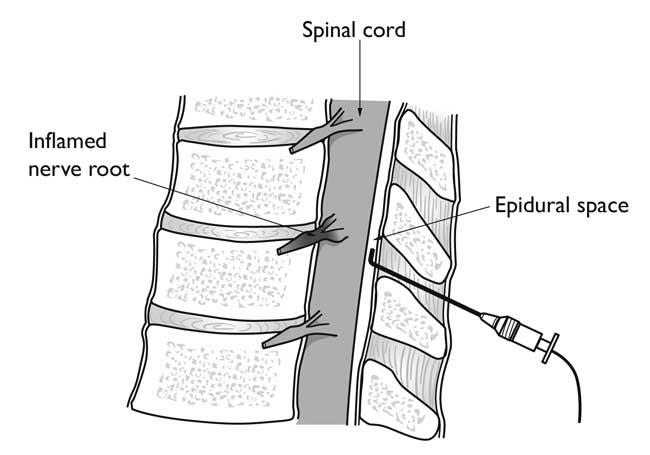
- Cervical epidural injections: In this procedure, steroid medication and an anesthetic is inserted into the space next to the covering of the spinal cord. This is called the epidural space and these injections are typically used for neck or arm pain that may be due to a disc herniation or bone spurs resulting in pinched nerves. This bathes the nerves in anti-inflammatory medication that can relieve symptoms.
- Cervical facet joint blocks: In this procedure, steroid and anesthetic medicine is injected into the small facet joints in the back of the spine. When these joints develop arthritis they may contribute to neck pain.
- Medial branch block and radiofrequency ablation: In certain cases of chronic neck pain, this procedure can be used to diagnose as well as sometimes treat a painful arthritic joint in the neck. In order to obtain a diagnosis, your doctor may block the nerve that supplies the facet joint in question with a local anesthetic. If your pain is relieved by this block, then your doctor may have pinned down the source of your neck pain! The next step which is a treatment option may be to permanently block that nerve with a “burning” technique called radiofrequency ablation.
Surgical treatment
Surgical treatment is not commonly recommended for cervical spondylosis and neck pain unless your doctor has determined either that:
- A nerve exiting your spine is being pinched in its channel by a herniated disc or bone spur and is contributing to your symptoms. Or –
- Your spinal cord is being compressed.
Patients who have neurological symptoms such as arm pain/weakness, numbness, or balance problems are more likely to be helped by surgery. That being said, surgery may also be an option if you have severe neck pain that has not been relieved by conservative measures and an exact pain generator can be identified by a combination of your physical exam and advanced imaging tests. Some patients with severe neck pain will not be candidates for surgery if the exact pain generator cannot be found. This could be due to the arthritis being widespread in nature or because of other medical problems or causes.
Key Takeaways
- Neck pain is common and often multi-factorial.
- The most common cause is degenerative changes that occur with aging, but can also be due to issues with nerves, tendons, muscles, and joints. The complex anatomy in the neck region sometimes makes finding the exact cause very difficult.
- Most patients with neck pain due to spondylosis (arthritis) experience stiffness and pain with motion. However if nerves are also being pinched can experience other symptoms.
- Conservative treatments are the mainstay of care for patients with neck pain due to cervical spondylosis.
- The optimal treatment regimen may involve a combination of therapies, medications, and injections and will be determined by you and your doctor on an individual basis.